by Craig Klugman, Ph.D.
A few months ago, I was attending a conference where the keynote speaker introduced herself as a bioethicist. She has never worked in a hospital setting; she has never performed consults; she has not written for the academic literature; nor has she taught a class. Her job was being a journalist, reporting on health and medicine. I was stumped as to why she called herself a bioethicist. In fact, one could argue that the job of a journalist is about reporting facts and events, not offering moral arguments and taking positions. I found my answer in her biography, she earned a master in bioethics in 2017.
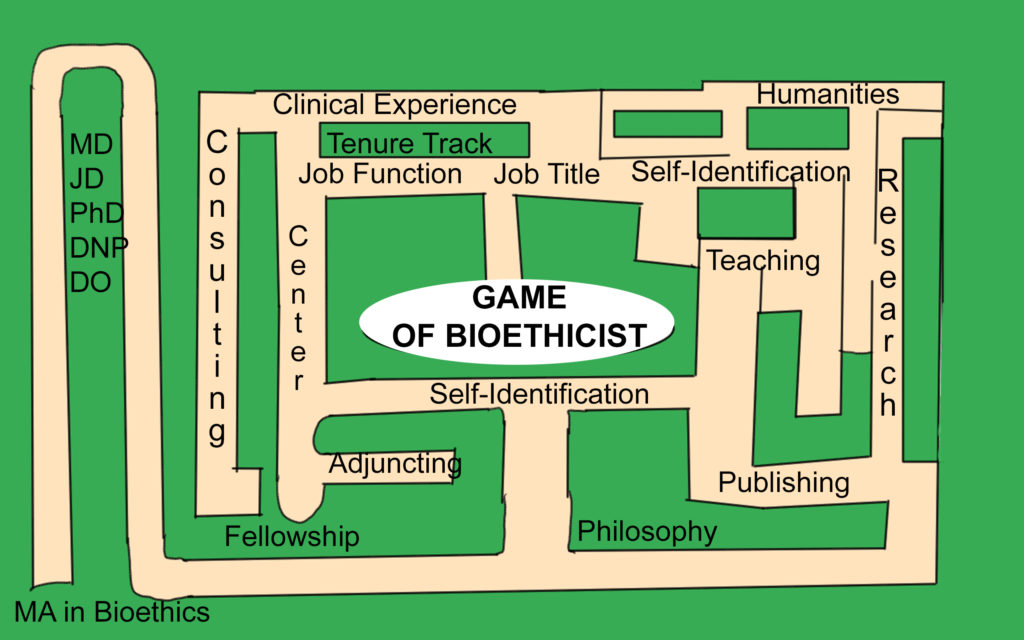 Later this week I am meeting with a student who has recently graduated with a doctorate in English and wishes to pursue an academic career in bioethics. These two events, two months apart have forced me to consider the question of what does it take to be a bioethicist? Is being a bioethicist simply holding a degree; working in a job with a set of tasks; a desire to do certain work; a set of trainings; or something else?
Later this week I am meeting with a student who has recently graduated with a doctorate in English and wishes to pursue an academic career in bioethics. These two events, two months apart have forced me to consider the question of what does it take to be a bioethicist? Is being a bioethicist simply holding a degree; working in a job with a set of tasks; a desire to do certain work; a set of trainings; or something else?
Although not a great resource, when exploring a broad question, it can be useful to get a sense of the popular perspective on the topic. According to Wikipedia, “Bioethicists are concerned with the ethical questions that arise in the relationships among life sciences, biotechnology, medicine, politics, law, and philosophy.” This is a definition by interest, anyone who is interested in these relations is a bioethicist. Notice that this is an inclusive, not an exclusive definition: Not everyone who shares these interests will identify as a bioethicist. Such a definition may describe much of the topical work, but it does not describe the settings, skills, training, or preparation necessary for this work. Is simply an interest in bioethical issues sufficient to be a bioethicist?
As the keynote speaker suggested, is having a degree in the field enough to call oneself a practitioner? After all, between 2000 and 2013, over 2,300 people earned advanced degrees in bioethics/applied ethics, including over 1,700 masters degrees. This perspective makes the assumption that the degree is part of a defined career-track and serves as an entry to practice. For example, most public health jobs require an MPH degree, thus an MPH is considered a practical degree rather than an academic one (defined as preparing one for research and teaching careers; pursuing knowledge for its own sake). MD, DNP, DO, JD degrees are part of a specific career track. However, just having the degree may not be enough, to be a medical doctor one must also complete a residency and attain a license. To be an attorney one must also pass the bar exam. However, without the degree, one cannot work in the profession. Bioethics is different. A masters in bioethics does not prepare one for a specific career path or profession, any particular training program, nor for an exam or licensure. A bioethics masters is not required to work in the field, and working in the field is not limited to people with a masters in bioethics.
The scholars who founded what is now called “bioethics” and who work as “bioethicists” do not have degrees in bioethics. They come from other disciplines and choose to work in this field. Should Art Caplan, Millie Solomon, Jim Childress, Dan Beauchamp, R. Alto Charo, Tom Murray, Ruth Faden, and many others no longer be called “bioethicists” simply because they lack a degree with “bioethics” in the title? In the early decades of the field, many scholars refused to be identified as “bioethicists” but rather were “philosophers,” “psychologists,” “physicians,” “theologians” with an interest in bioethical issues. Clearly the founders and luminaries of the field should not have this label removed because of lack of a specific degree. Besides, there is no one defined or determined curriculum that underlies the bioethics masters degree. These programs vary in terms of what philosophers are taught, what core readings are read, what methods for clinical consultation are preferred, and even what constitutes the work of bioethics. Thus, simply having a master’s degree in bioethics does not make one a bioethicist.
Perhaps being a bioethicist is simply about where one does the work. If you work in a bioethics center or with the title of bioethicist (even lacking any training), then perhaps the term applies. For example, I had an MD colleague who had no background, no degrees, no reading, no experience, and no interest in learning about bioethics but by virtue of leading a bioethics center, thought that they should be called a “bioethicist.” This would be a definition by affiliation. I felt differently and thus never referred to them as such, a point that did create tension in our working relationship. In all honesty, although I spent 5 years working in an academic medical center, interviewing prospective students, researching, teaching, developing curriculum, and clinical consulting, I never asked anyone to call me “physician” simply because of the location where I did my work.
Under the ASBH Clinical Ethics Consultation Affairs (CECA) committee credentialing pilot program, a clinical ethicist needs to have an advanced degree, clinical experience (i.e. fellowship or substantial work experience), and have a portfolio of case—For more information, see Improving Competencies in Clinical Ethics Consultation, second edition. Some scholars have pointed to the need for CECA as arising out of this very issue: Given a lack of definition and criterion for being a bioethicist (in the case of CECA, a clinical ethicist), anyone can take on the label irrespective of their training, background, and skillset.
A 1999 article in The Scientist explored the career path of bioethicists. The article interviewed many notable names who suggested that bioethics is not about the disciplinary training but more about the areas of study and location of one’s work. The author writes about the growing number of bioethics degrees, suggesting there could be a change forthcoming in training paths. The bottom line in this essay is that a higher degree is necessary, but not sufficient.
The career webpage at the Berman Institute (Johns Hopkins) offers stories of the faculty and how they found bioethics. The same page suggests places where people in bioethics work: “academic bioethics” including universities and think tanks, “research ethics,” “clinical ethics,” and “be creative…. don’t be afraid to be creative in encouraging the integration of bioethics into existing career paths. Some obvious examples: cell biologist-bioethicist, NICU nurse-bioethicist, historian-bioethicist, hospital administrator-bioethicist.” The instructions here suggest what I usually tell my students interested in bioethics careers:
- Unlike medicine and other clinical health careers, there is not a defined career path to follow
- A masters in bioethics can be a great experience, but it’s not enough: You need to have a terminal degree
- Similar to what the Berman Institute hints at, think of your bioethics masters degree as a value-added proposition—it provides a new way of viewing the work that you already do or are already prepared to do and may open some doors within your existing work (such as serving on an IRB, IACUC, or ethics committee)
- Like medicine, bioethics cannot be learned solely from books but one must participate in research, clinical consultation training, internships/fellowships in hospitals, and publishing/presenting
This analysis leads back to the original supposition: Is the bioethicist one who holds a degree, holds a title, works in a bioethics center, publishes in bioethics journals (though much bioethics is published in science, medicine and social science journals), teaches courses in bioethics, conducts research, works in a research or medical environment, provides ethics consulting, or simply declares that he or she is a bioethicist? The reality is that there is no definitive answer. As a field, we have avoided defining what is a bioethicist in an attempt to be as inclusive as possible, given our varied beginnings. The problem, of course, is that anyone can grab the title and represent what we do even if they have no idea what it is that we do. I propose that a bioethicist is someone whose core professional identity and activities is in doing bioethics. Thus, this not the person who is a journalist who has studied bioethics; nor the nurse who serves on the ethics committee. Rather this is the bioethicist who also writes for a news outlet and a clinical bioethics consultant who also has some nursing responsibilities. In this way, the self-identification is maintained, but the person must have the background, experience, and position where doing bioethics is their primary work.
Returning to my initial prompts in thinking about the keynote speaker and the recent graduate, given the lack of definitions and criterion for being a “bioethicist” there is no way to prevent someone from self-identifying as such. However, I should have spoken to the journalist and suggested that she refrain from taking on that title simply for completing a degree. I do not doubt her masters may have helped her work in journalism, but writing about bioethics or about medicine does not make one a bioethicist. Of course, she could argue that I am not the arbiter of who is and what makes a bioethicist. And she would be correct.
For the English graduate, I may suggest that he consider a bioethics masters or a fellowship program. I may even advise he look at medical/health humanities positions as opposed to those in bioethics since that viewpoint may better fit his interests and his credentials.
To paraphrase the U.S. Supreme Court in Jacobellis v Ohio, “I shall not today attempt further to define the bioethicist…and perhaps I could never succeed in intelligibly doing so. But I know one when I see one….”